Many thanks to Len Press for identifying this collection of articles on the neurological underpinnings of VISION and visual processing.
Dr. Press’ blog highlights this diagram from the article, Origins of Strabismus.
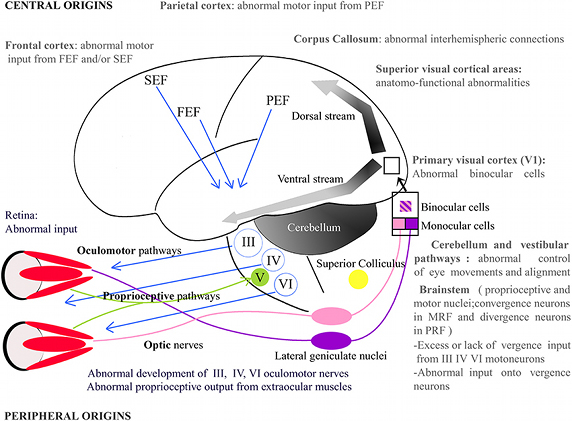
FIGURE 2 | Potential origins of strabismus. Strabismus may have sensory and/or motor origins as well as peripheral and/or central origins. In periphery, one may notice, for example, abnormal vision or abnormal development of the extraocular muscles. In the latter, the extraocular muscles’ proprioceptive afferents reaching the Gasser ganglion normally through the ophthalmic branch of the Vth (trigeminal) cranial nerve and/or their oculomotor nerves, i.e., the IIIrd, IVth, and the VIth cranial nerves, may be also altered. Centrally, strabismus may, for example, result from an abnormal activity in the brainstem, the Medial Reticular Formation (MRF), the Pontine Reticular Formation (PRF), the thalamus, the cerebellum or the superior colliculus. At the cortical level, visual, parietal or frontal cortex may also not function properly. Altogether, this indicates that origins of strabismus may be numerous. One may emphasize that those with a central origin likely dominate. FEF, Frontal Eye Field; SEF, Supplementary Eye Field; PEF, Parietal Eye Field; III, IV, V, VI: brainstem nuclei III, IV, V, and VI and their motoneurons.
When strabismus is diagnosed, it is on the basis of an external sign — eye misalignment. This article does a wonderful job of highlighting the myriad ways in which strabismus may develop in an individual. They note that “central nervous system” problems account for 95% of strabismus, while “peripheral origins,” localizing with the eye muscle development or dystrophy, account for only 5% of strabismus.
The take home: Strabismus is not just an eyeball or eye muscle problem!
And many articles in the literature are already identifying ways in which quality of binocular vision can be modified with perceptual training!


Leave a Reply